
|
|
John Stetson
|
John B. Stetson started a hat factory in Philadelphia in 1865, and within a few years, The Stetson was synonymous with cowboy hats. The quality was good, and the image was perfect for the migration into the West which took place after the Civil War, urged onward by that myth of the noble cowhand so enthusiastically nurtured by Philadelphia authors, books and magazines. From time to time, a Stetson hat could be seen on a Philadelphia head, but for the most part, Stetsons were more a factor in Philadelphia commerce than Philadelphia styles.

|
|
Stetson Hat Factory
|
The matter came up recently when someone by that name was asked if he belonged to the hat family, and it turned out that was so. In one of those brief cocktail party encounters, he remarked that what ruined the Stetson hat factory, was John Kennedy appearing at his presidential inaugural -- hatless.
Aside from the fact that young Kennedy's hatlessness did not seem to affect the Texas factory which still makes Stetsons, there is the recollection that hatlessness was pretty stylish fifteen years before the Washington Camelot, both in men and in women. In fact, hatless young women were a Philadelphia style for quite a while before they were a national style.
It seems reminiscent of another fable about changing styles, attributed to Clark Gable. The movie star took off his shirt in a movie called "It Happened One Night", revealing bare skin. Undershirts, one is to believe, promptly disappeared from American life. There are those who recollect that undershirts suddenly got hard to find during World War II, and were replaced by T-shirts by the armed forces. There is a strong odor of Publicity Agent about both of these clothing stories, but things have got fairly advanced when even members of the manufacturing family are now repeating the folklore.

|
|
American two-party system
|
America's two-party system took fifty years to stumble into permanence. Regardless of the happenstances of their eventual emergence, political parties were clearly not designed into the original plan. Those few founding fathers who did think about political parties rejected them as "factionalism", something to be condemned. The true nature and advantages of a two-party system began to be truly venerated when other nations tried something quite different, which we now call Proportional Representation. PR is a fairly natural outgrowth of creating a large democracy from a collection of little tribes -- then creating surrogate political parties for them as part of the design. Guided by historical experience, it is now possible to ignore all minor differences between stable two-party democracy and multi-party democracy, except one. In a two-party system, the political dealing and vote-swapping takes place before the election, with all the players jockeying and sacrificing principle to answer a single candidate question, "Can he win?" By contrast, in a multi-party or proportionally-represented democracy, the election comes first, and only subsequently do vote-swapping and artful promises construct the ticket of candidates and the policy platform. The plain fact is the public doesn't know whom it is voting for and often is disagreeably surprised. Furthermore, important matters remain unsettled by a multi-party election. A cabinet member of a splinter party, potentially one with negligible public support, retains the threat of resigning if things don't go his way, and his resignation may trigger a whole new national election if it breaks up the political margin of the ruling coalition. At least, a two-party system settles things for a while and gives the public a relative rest from factional tensions.
The American system has evolved into a universal conviction, stronger than any Constitution, that two parties are quite enough. Third parties are of course tolerated because they aren't forbidden, but most offer a mechanism in case there is a serious wish to reconstitute one of the two major parties. The strength of third parties is to discipline the leadership of the major parties; the weakness is they threaten the unifying principle of compromise-in-order-to win. Nothing except religious fanaticism would likely induce any ambitious American politician to remain within a third party, fruitlessly frittering away his life's chances. Because of 18th Century history more than wisdom, an "established" religion is constitutionally prohibited in America; observation of the turmoils in other nations, and perhaps wisdom also, keep it that way.
If two parties are then quite enough, is it possible only one would be better? The quickest look abroad, the briefest exposure to history, shows a one-party system is synonymous with dictatorship. Communism and fascism had only this one feature in common; in fact, China seems to be morphing from one to the other, while resolutely retaining its single ruling-party system. The paradox of this situation is that it leads to the American realization that maintaining a two-party system means that neither party must ever achieve total victory. After each national election, the electorate settles back with relief that one side won, but neither side conquered. Even academics are muffled by the system; with much to criticize, there is nothing else worth substituting.
There is one thing left to mention about the two-party system, which is that the interests and affiliations which arouse the club-like loyalties of party members seldom perfectly match the party's current campaign policy issues, and depend in a high degree on habit and a formless sense of group comfort. Any schoolchild can notice, although the party candidates avoid mentioning, that policy issues move back and forth between the two parties. Whether it is tariffs, public schooling, the gold standard or a thousand other matters, the issues repeatedly shift to the other party when lack of progress or apparent betrayal offends them. The special interests seek to use the parties, and the parties regard each special interest as a bargaining chip; the gut feelings of the party membership adjust far more slowly. For maximum effectiveness, a two-party system needs the public to see itself as two warring affinity groups; for a while, polarization seemed to revolve around the rich and the poor. There would always be more poor people than rich ones, as the Founding Fathers feared and the anti-Federalists sought to exploit; but now Populism can only be sustained by continuous massive immigration. The times are growing stale for the Republicans to suggest that only they have an electoral incentive to eliminate poverty, while the Democrats would secretly like to increase it. Or for the Democrats to imply they have a monopoly of sympathy for the poor. Compared with the status of the rest of the world, permanent lifetime poverty in America is growing too infrequent to dominate elections, even supplemented by fear of poverty, a recollection of having once been poor, or guiltiness about never being poor. It is difficult to maintain the firmness of party members with such vague attitudes for abstruse legislative policies like banking reform or compulsory health insurance. Therefore, the search is on for large social affiliations which would more comfortably enlist loyalties for pressing specific legislative actions. At the present time, division of the working populace into the public and private sectors is being promoted as a bedrock political affiliation, but it is questionable whether that will be as successful as the public sector unions seem to hope for. Only twice in our history, during the administrations of George Washington and James Monroe, have Americans overwhelmingly agreed on core issues of religion, foreign policy, and prospects for the future. During both episodes, political parties virtually disappeared.

|
|
Henry Cadbury
|
There are a few old Quaker Clothes in the attics of their descendants, and on suitable occasions, an old broad-brimmed hat or two will appear at a Quaker gathering, for amusement. Quakers gave up the old style of "plain dress" when it became generally agreed that such eccentric dress was not plain at all but rather drew attention to itself. On the other hand, there is a distinctly unfashionable quality to almost everything Quakers do wear. When silk and nylon stockings were fashionable for women, Quaker women often wore black stockings. When it became the style for women to sport black stockings, Quaker women usually wore flesh-colored nylons. Among men, thin metal-trimmed spectacles displayed the same counter-fashionable tendency. Nowadays, these little quirks are often public signals among strangers, a way of wig-wagging "I notice you are a Quaker, so am I." And of course, unfashionable clothes are cheaper, and that's always a good thing.
And so it happened in 1947 that the Quakers were awarded the Nobel Peace Prize, with information passed along that white tie and tails were the expected form of dress at the ceremony. Henry Cadbury was selected to receive the award on behalf of the American Friends Service Committee, and you can be sure Henry Cadbury didn't own a set of tails. Henry was also very certain he wasn't going to go out and buy a set, just for a single wearing.
The AFSC collects used clothing, to distribute to the poor. Henry inquired whether there might be a set of white tie and tails to be found in the used-clothing bin, and luckily there was. It had been collected on behalf of the Budapest Symphony Orchestra when that impoverished but distinguished group of musicians was invited to give a concert in London. One of the monkey suits more, or less, fit Henry.
So, after investing in dry cleaning and pressing, Henry packed it up and went off to Oslo, to meet the King.

|
|
Septa
|
Byron S. Comati, the Director of Strategic Planning and Analysis for SEPTA (Southeastern Pennsylvania Transportation Authority), kindly gave the Right Angle Club an inside look at the hopes and plans of SEPTA for the near (five-year) future. Students of large organizations favor a five or six-year planning cycle as both short enough to be realistic, and long enough to expect to see tangible response. If plans continuously readjust to fit the five-year horizon, the concept is that the organization will move forward on these stepping stones, even accounting for setbacks, disappointments, and surprises. Furthermore, a serious level of continuous planning puts an organization in a position to react when funding opportunities arise, such as the sudden demand of the Obama Administration that economic stimulus proposals be "shovel ready."

|
|
The Silverline V
|
So, SEPTA is currently promoting five major expansions, based on the emerging success of an earlier plan, the Silverliner V. Silverline is a set of 120 shiny new cars, built in Korea on the model of electrical multiple units, which are expected in Spring 2011 to replace 73 cars or units which were built in 1963. Obviously, 120 are more expensive than 73, but they are more flexible as well. And less wasteful; most commuters are familiar with the model of three seats abreast which unfortunately conflict with the social preferences of the public, tending to make the car seem crowded even though it is a third empty. When a misjudgment like this is made, it takes fifty years to replace it with something better. For example, there's currently a movement toward "Green construction", which is acknowledged to be "a little bit more expensive". The actual costs and savings of green construction have yet to become firmly agreed on, so there's an advantage to being conservative about what's new and trendy in things that take fifty years to wear out.
|
|
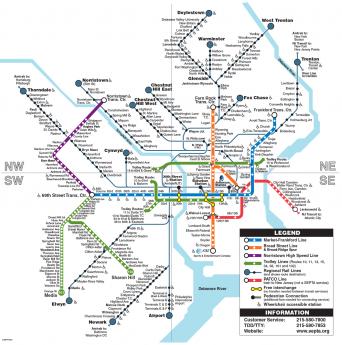
Septa Regional Map
|
Four of SEPTA's five major proposed projects are in the Pennsylvania suburbs. New Jersey has its own transportation authority, and Philadelphia is thus left to struggle with the much higher costs of urban reconstruction assigned to its declining industrial population. And left unmentioned is the six hundred pound gorilla of the transportation costs of new casinos. A great many people are violently opposed to legalized gambling, and even more upset by the idea of crime emerging in the neighborhoods of gambling enterprises. Even the politicians who enacted this legislation are uncomfortable to see the rather large expenditures which will eat into the net revenue from this development. Nevertheless, if you are running a transportation system, you have an obligation to plan for every large shift in transportation patterns, no matter what you might think of the wisdom of the venture. The alternative is to face an inevitable storm of criticism if casinos come about, but without any preparation having been made for the transportation consequences. At present, the public transportation plan for the casinos is to organize a light rail line along the Delaware waterfront, connecting to the rest of the city through a spur line west up Market Street; it may go to 30th Street Station, or it may stop at City Hall. That sounds a lot like the present Market-Frankford line, so expect some resistance when the cost estimates are revealed. Because all merchants want to have the station stops near them, and almost no residents want a lot of casino foot-traffic near their homes and schools, expect an outcry from those directions, as well. It would be nice to integrate this activity with something which would revive the river wards, but it seems a long stretch to connect with Wilmington on the south, or Trenton on the north.
The planned expansions in the suburban Pennsylvania counties will probably encounter less controversy, although it is the sorry fate of all transportation officials to endure some hostility and criticism for any changes whatever. Generally speaking, the four extensions follow a similar pattern of building along old or abandoned rail lines, following rather than leading the population migrations of the past. When you are organizing mass transit, there is a need to foresee with some certainty that there will be a net increase in commuters in the region under consideration. The one and two passenger automobile is a much more flexible instrument for adjusting to the growth of new development, schools, retail, and industry. Once the region has become established, there is room for an argument that transportation in larger bulk is cheaper, cleaner or whatever.
The Norristown extension follows the existing but underused rail connections to Reading. Route US 422 opened up the region formerly serving the anthracite industry, but now the clamor is rising that US 422 is impossibly crowded and needs to be supplemented with mass transit.
The Quakertown extension follows the rail route abandoned in 1980 to Bethlehem and Allentown, although the extension is only planned as far as Shelly, PA.
The Norristown high-speed extension responds to the almost total lack of public transportation to the King of Prussia shopping center, and will possibly replace the light rail connection to downtown Philadelphia.
And the Paoli extension follows the mainline Amtrak rails as far as Coatesville.
All of these expansions can expect to be greeted with huzzahs by developers, land speculators, and newsmedia, but resistance will inevitably be as fierce as it always is. Local business always fears an expansion of its competitors; the feeling is stronger in the suburbs than the city, but local business always resists and local politicians always follow their lead. To some extent, the suburbs have a point, since radial extensions are usually much cheaper to build than lateral or circumferential transportation media; bus routes are the favored pioneers in connecting one suburb with another. Therefore, the tendency in these present plans remains typical by threatening the suburbs with a need to travel toward the center hub, then take a reverse branch back in the general direction of where they started, in order to go a short distance to a shopping center or school system. The two main river systems around Philadelphia interfere with the construction of big "X" routes from the far distance in one direction to the far distance in the opposite direction. Euclidian geometry makes the circumferential route elongate as the square of the radius. And jealousies between the politicians in three states create rally foci for the special local interests which feel injured. Since it seems to be an established fact that the proportional contribution to mass transportation by the surrounding suburbs of Philadelphia is traditionally (and considerably) lower than the national average, a political reconciliation might do more for the finances of SEPTA than any federal stimulus package could do. For such reconciliation, a few lateral connections in the net might pacify the suburbs enough to justify the extra cost. Unfortunately, the main source of unjustified cost in regional mass transit is the high wage and benefit levels of the employees, a situation inherited from the old days when commuter rail was part of the stockholder-owned regional railroads. Just as featherbedding was the main cause of the destruction of the mainline railroads, health and pension benefits threaten the life of mass transit. In the old days, local governments acted as a megaphone for union demands. So the railroads just gave the commuter system to the local governments, and let them wrestle with the unions themselves. Since the survival of the urban region depends on conquering this financial drain, the problem must be gradually worn down. But it has been remarkable how long the region has been willing to flirt with bankruptcy rather than bite this bullet.
If anything, this friction threatens to get worse. In 2009, for the first time, a majority of union members in America -- work for the government, the one industry which thinks it cannot be destroyed by losing money. True, SEPTA is not exactly a government function, but it has enough in common with a government department to arouse suburban voters, who regularly refer to it as an arm of the urban political machine. SEPTA isn't too big to fail, but there exists little doubt that government at some level would probably try to bail it out if it did.
If the United States Supreme Court makes a mistake, it remains pretty much a mistake in residence until the Court itself re-examines the matter. It would be indelicate for anyone else to cite a list of examples for this observation, so they are customarily taken up one at a time, at considerable expense. The desirable re-examination with the greatest consequence to Healthcare would be the 1982 decision in State of Arizona v. Maricopa County Medical Society.
Maricopa County is where Phoenix is located in Arizona, and its County Medical Society was one of the pioneers in what was then called Foundations for Medical Care. These were organizations in which local physicians took the lead in organizing and managing health insurance for the local community. The rules and policies of the Foundations were conceived and implemented by physicians, who were dismayed by the consequences of defects in health financing they could see in daily practice. Except for this physician dominance, it would be fair to say that Foundations for Medical Care were about the same as what we now call HMOs. It is also true these physicians were impatient with both the government and the health insurance companies, who seemed to resist helping the sick poor by implying it might violate some per se technicality aimed at business corporations. As the lame excuse would have it, our hands are tied. The obvious fact is someone in Arizona didn't like physicians or didn't like what they were threatening to do.
An agreement among competitors to lower prices for the poor, is after all not exactly the same anti-competitive behavior, as a "contrivance" to raise prices for your own benefit. It seemed most unfortunate to lump it together with its opposite as "per se" violations, requiring no examination of the evidence to distinguish the two. And furthermore, on the topic of regulating business corporations, it is not exactly an enumerated Constitutional power of the federal government, to amend the Constitution by treating all corporations as essentially identical or lowering prices the same as raising them. The whole anti-Foundation movement sounds pretty spurious.
At the same time, "Foundation" physicians believed they could see opportunities for reducing waste in the local hospitals which would only be exploited if physicians were in charge because physicians could sense the cost/benefit more readily than anyone else. Having recently returned from the Korean War, these doctors knew medical care could be excellent even without such a thing as health insurance, and indeed even if hospitals were only a collection of tents. Perhaps a few of them were overly influenced by the TV serial, "MASH", whose central theme is that if doctors take the lead and do the right thing, much can be forgiven. That's a sort of Hollywood restatement of the latitude of ancient Courts of Equity, charged with finding a way to achieve Justice --to cover a situation where obvious harm exists, but no law exactly addresses it.

|
|
|
Accordingly, the "better sort" of the doctor in Arizona believed they perceived the respectable doctors would readily agree to care for the poor at lower rates, whereas the shirkers in their midst would ruin things for everybody by refusing to do a fair share of pro bono work. Like labor unions, the doctors greatly resented the free rider phenomenon.
The idea of a two-class system of medical care was also abhorrent to them, however; if there wasn't enough money to spread around, a "good" doctor would just agree to lower his fees unilaterally. This moral quarrel often conflicts American business, which takes the view that it doesn't really matter what costs or taxes or burdens are imposed by the government. What matters to big business is that all competitors need to abide by the same handicaps. When handicaps are roughly equal, the difference between success and failure is -- talent. But the contrast between that and the antitrust position of individual tradesmen has never been satisfactorily defined.
To a considerable degree, talent rising to the top summarizes the aspirations of the anti-trust statutes, where it regularly becomes a source of both suppression and escalation of prices. Physicians are ultimately expected, not least by their colleagues, to find their highest duty is fiducial to the patients' best interest, particularly when the main conflict is merely a financial one. A corporation, by contrast, has a primary duty to its shareholders, who can sue them if they put benevolence ahead of profit. A corporation is a contract between the State and the shareholders, quite the reverse of the duty of government to its individual citizens. In the antitrust arena, the contrast between citizen and corporation is jumbled. Particularly in the case of the per se violations, the difference between a business corporation and a medical society is quite wide enough to justify considerable professional latitude. As it is not, in the case of insurers, and as it only partly remains, in the case of hospitals. Anti-trust statutes could have a real value in distinguishing borders between individual tradesmen and various groupings of them, but so far the distinctions are far from reasonable. The Maricopa Medical Society responded with perhaps excessive enthusiasm to the challenge of making local sense out of a price-fixing dilemma, but it was never given the opportunity to make its case.
At one time, local healthcare costs were suppressed by imposing competition on the hospitals, holding insurance administrators to be mindless clerks to pay the bills, not as cup-bearers of fairness in a naughty world. Needless to say, the hospitals and health insurers had long chafed at the ability of physicians to switch hospitals freely, and the patients to switch insurers, whereas Arizona's Attorney General seemed to suspect some vague return to Robin Hood notions of a special right to defy the law. Somehow the ancient concept of professional latitude has been supplanted as inconvenient to the goals of competitors. In certain parts of the country, big business is already expanding its financial control of hospitals and insurers, into acting as agents for assuring high-quality medical care, while suppressing its cost. On Wall Street, such behavior is quickly seen and labeled as "talking up your book of business". With the defeat of physicians by the Maricopa decision, plus the withdrawal of big business owners from identifiable management roles, the way was soon opened for hospitals and insurance companies to assert unrestrained control of their own finances. Thirty years later, hospitals and insurers are now universally merging, and applying selective controls over admitting pliant physicians as their employees. The Affordable Care Act is the mechanism by which the government interjects a new layer of control, thereby converting the government itself into the new hidden battlefield. It seems a very far cry from leaving medical decisions in the hands of physicians and their patients, to choose treatments, and to agree on their price.

|
|
Sen. John Sherman
|
The Attorney General of Arizona, himself a colorful character, soon brought suit for an anti-trust violation, since price-fixing was a declared per se violation or identification of the absence of competition. These were additions made to the Sherman Anti Trust Act by earlier Supreme Courts, who found an Act first written on the back of an envelope was lacking in regulations. Further strictures were imposed by the Clayton Anti-Trust Act, but these both might be remedied by subsequent Congresses, and thus lacked appropriate majesty. The crucial consequence was that the District Court of Arizona found it quite unnecessary to hold a trial or hear the evidence. The Court found against the doctors entirely on the basis of a motion for summary judgment. The matter then passed through the Court of Appeals to the Supreme Court, which on the theory that price fixing is price fixing, on a vote of 4 to 3, upheld the Arizona suit. All the way from a writ of summary judgment in a district court, to the United States Supreme Court, without formal examination of the facts. If either of the two absent members eligible to vote, had voted, it is certainly mathematically possible for the decision to have gone the other way.
Perhaps, strictly on lawyerisms, that was safely correct. But in terms of the effect on medical care, it won the war for control of hospitals and the insurance companies which began with Abraham Flexner's beatification of college-educated physicians. Somehow Maricopa was interpreted to mean that a hospital or an insurance company might do many medical things which were forbidden to organizations run by physicians. The consequence is Foundations run by physicians are under constant threat of what might happen to them if they do what HMOs are now seen to be doing every day. The whole Clinton health fracas revolved around this particular case and its implications. From the physician point of view, if you had medical training, you had been disqualified from running a Health Maintenance Organization, because a change of leadership seems to shift the antitrust issue to a different level within two identical organizations. And that was true even if the physician had been trained for the role, while the administrator had not.
What was particularly galling was to be tarred with the brush of antitrust, whereas others could describe identical behavior as self-disciplined and in the public interest. Self-imposed financial restraint was taunted and abused by aspirants for the same job with the same temptations, with multi-million dollar incomes, but without adherence to the same code of ethics. The emerging joke is that after the Clinton Healthcare Plan's uproar, the public decided they disliked HMO's intensely, mainly because they couldn't choose their own doctor, and the doctor was being hampered in doing what seemed professionally best for the patient. None of these legal issues had significantly arisen for physician-run HMOs. While of course, that outcome might appear, such disputes would be settled by physicians, using medical arguments, followed by a change in management if the medical community at large, widely disagreed with the decision. The only substantial difference was that doctors were running one organization but subservient in the other, and the Courts had found that whenever doctors were in charge it amounted to price-fixing between competitors. As matters eventually turned out, the hospitals resolved this battle by converting nearly all practicing physicians into their employees, and the war has now shifted to who will control hospitals.
It now remains for some case to be found and carried to the Supreme Court which might allow an examination of the facts of this matter, perhaps remanding the case back to the District Court to hold a trial. That would seem a bare minimum after thirty years, even though now it might no longer address precisely the same issue. Somehow, a way must be found to examine which of two rather extreme theories of the Wild Wild West needs to be laughed off. Either we must re-examine whether, always and everywhere, price-fixing is such an undiluted evil it never requires an examination of the evidence. Or whether the absence of identifiable harm introduces a balancing need to question such judgments when made under professional circumstances.
While on the subject of mixing business practices with professional standards, we might as well direct judicial attention to the unfair and probably (equal justice) unconstitutional tax preference for employers who purchase health insurance for their employees, to enjoy a huge corporate tax saving themselves by doing so. Not merely for the benefit of the employees, which is much discussed, but a usually much greater financial benefit for the shareholders when the corporate tax level is high enough. An unnecessary grievance is created for millions of self-employed and unemployed people who lack this tax shelter, and also for the owners of usually much smaller business enterprises, who must compete with them.
It might be argued that double taxation of corporations inevitably provides the loophole of double tax-exemption, and even this would often understate the discrepancy because of the differences in marginal rates. Lack of participation in this double tax benefit is arguably the main obstacle to extending employee health insurance to others or even substituting a superior health payment methodology. Now seventy years old, this grievance can be regarded, not only as having dubious evasions at its historical origin, but has resisted multiple efforts for repeal, and distorts the relative lifestyles of the two main participants in the workforce: small, and large, businesses. Henry Kaiser claimed he once had difficulty attracting employees to his West Coast war industries because of wartime wage and price controls, an excuse which should have ended the practice in 1945. Lack of a review-and-reconstruction of this bizarre lobbying product could potentially distort the application of the Affordable Care Act, in ways which are impossible to foresee. Indefinite enshrinement of the legal principles in this tangle, particularly the indefinite postponement of its resolution, could reverberate for more decades. The fringe-benefits circumvention, for example, has since grown entirely out of control, while it is fiercely defended by business and union interests. As it grows, however, the inequity to the self-employed and unemployed by remaining excluded from it, also grows.
Summary of the Maricopa Case
From a legal standpoint, the most uncomfortable feature of the case of the Maricopa Medical Society is that it went all the way to the Supreme Court without any trial of the facts or real opportunity for the defendants to present their case. That is, the whole HMO movement was effectively removed from the hands of physicians by a motion for summary judgment, on a Supreme Court decision, 4 to 3. It would be interesting to learn the attitudes of the remaining two Justices who recused themselves, but who could have reversed it.
To hold a trial of the facts by remanding the case for trial, would seem to be one easy way to introduce the defense which the doctors would have made. It could be improper to suggest to their lawyers what the defense should now be because new officers of the Medical Society might hold different opinions. The Medicaid Act was passed in 1965, requiring state consent for a jointly administered program. By 1972, Arizona was the only remaining state not to have agreed to Medicaid, which by then was widely recognized as the worst run and most underfunded medical program in America. In 1982, Arizona adopted a small portion of Medicaid, and it was only in 1988 that it fully adopted the program. In 2001, Arizona's governor was offered 7.9 billion dollars over four years, as matching money for the insurance exchange feature of the Affordable Care Act, which by then heavily absorbed the Medicaid program. The Governor recommended to the Legislature that they accept the offer because at least it was "better than Medicaid". There can be little doubt the Legislature of Arizona was adamant on the issue. And the Medicaid program is certainly better funded than it formerly was. But the central feature of Medicaid's HMO remains that of the Maricopa decision: its policies and administration are not directed by physicians. On the issue of whether the control should rest with payers or professionals, payers prevailed.
What were the doctors expected to do with sick poor people? No doubt, there was a wide divergence of opinion, but it must have seemed likely to someone, only a handful of saintly volunteers would now step forward, and none of them would be willing to pay hospitals their list prices. There is some truth to the last part. The doctors felt it would only work by shaming a substantial majority of their own members into accepting the cases at discount prices, and the only weapon they had was to make it a condition for membership in the medical society. That might once have been a powerful incentive, but the systematic undermining of its powers has now made it more questionable whether it could still succeed in its original plan. At the time of the first trial, there was probably enough slack in hospital revenue to cover the indigent need. With a changing economy, the premise needs to be tested more hesitantly.
Under these contentious circumstances, surely the Supreme Court could, even now, find some words to devise a better outcome. Price fixing is a per se violation of the act, and there is little doubt that all HMOs now fix prices. Only a physician-run HMO can be accused of "fixing" prices too low for competitive reasons, although it has always been arguably how strongly they would naturally compete for indigent patients. The Supreme Court may be reluctant to overrule the price-fixing part because of the spill-over effect of a century of custom, and the Arizona politics of this case are surely thorny.
As time passes, the Maricopa case is fast becoming as dignified by long-standing, as the price "fixing" notions were when it all started. Surely, at least the Court could find some clarifying language about physician-run HMOs as obiter dicta . The response of the non-physician-run HMOs was to exploit the opportunity to eliminate the competition of physician-run groups within the price-fixed arena. In the meantime, however, the public has found HMOs run by non-physicians have become contentious in the extreme, whereas the earlier physician-run Foundations for Medical Care were tolerated by most physicians, and embraced by quite a few. The matter is one of the important threads in the Obamacare controversy, so the Supreme Court has an opportunity to improve quite a few situations by writing a clarifying paragraph or two.


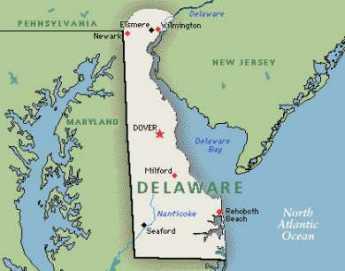 Originally the "lower counties" of Pennsylvania, and thus one of three Quaker colonies founded by William Penn, Delaware has developed its own set of traditions and history.
Originally the "lower counties" of Pennsylvania, and thus one of three Quaker colonies founded by William Penn, Delaware has developed its own set of traditions and history.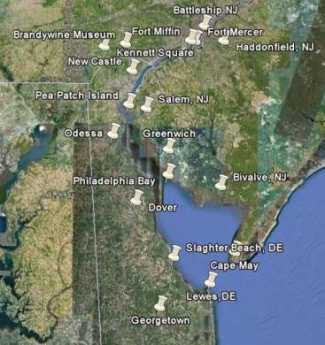 Start in Philadelphia, take two days to tour around Delaware Bay. Down the New Jersey side to Cape May, ferry over to Lewes, tour up to Dover and New Castle, visit Winterthur, Longwood Gardens, Brandywine Battlefield and art museum, then back to Philadelphia. Try it!
Start in Philadelphia, take two days to tour around Delaware Bay. Down the New Jersey side to Cape May, ferry over to Lewes, tour up to Dover and New Castle, visit Winterthur, Longwood Gardens, Brandywine Battlefield and art museum, then back to Philadelphia. Try it! Millions of eye patients have been asked to read the passage from Franklin's autobiography, "I walked up Market Street, etc." which is commonly printed on eye-test cards. Here's your chance to do it.
Millions of eye patients have been asked to read the passage from Franklin's autobiography, "I walked up Market Street, etc." which is commonly printed on eye-test cards. Here's your chance to do it. In 1751, the Pennsylvania Hospital at 8th and Spruce was 'way out in the country. Now it is in the center of a city, but the area still remains dominated by medical institutions.
In 1751, the Pennsylvania Hospital at 8th and Spruce was 'way out in the country. Now it is in the center of a city, but the area still remains dominated by medical institutions. Grievances provoking the American Revolutionary War left many Philadelphians unprovoked. Loyalists often fled to Canada, especially Kingston, Ontario. Decades later the flow of dissidents reversed, Canadian anti-royalists taking refuge south of the border.
Grievances provoking the American Revolutionary War left many Philadelphians unprovoked. Loyalists often fled to Canada, especially Kingston, Ontario. Decades later the flow of dissidents reversed, Canadian anti-royalists taking refuge south of the border.







